Medical Center » About Us » Patient Safety and Quality » Central Line-Associated Bloodstream Infections (CLABSI)
A central line is a catheter (tube) that doctors often place in a large vein in the neck, chest, or groin to give medication or fluids or to collect blood for medical tests.
You may be familiar with intravenous catheters (also known as IVs) that are used frequently to give medicine or fluids into a vein near the skin’s surface, usually on the arm or hand, for short periods of time. Central lines are different from IVs because central lines access a major vein that is close to the heart and can remain in place for weeks or months and be much more likely to cause serious infection. Central lines are commonly used in intensive care units.
A central line-associated bloodstream infection (CLABSI) is a serious infection that occurs when germs (usually bacteria or viruses) enter the bloodstream through the central line. Healthcare providers must follow a strict protocol when inserting the line to make sure the line remains sterile and a CLABSI does not occur. In addition to inserting the central line properly, healthcare providers must use stringent infection control practices each time they check the line or change the dressing. Patients who get a CLABSI have a fever, and might also have red skin and soreness around the central line. If this happens, healthcare providers can do tests to learn if there is an infection present.
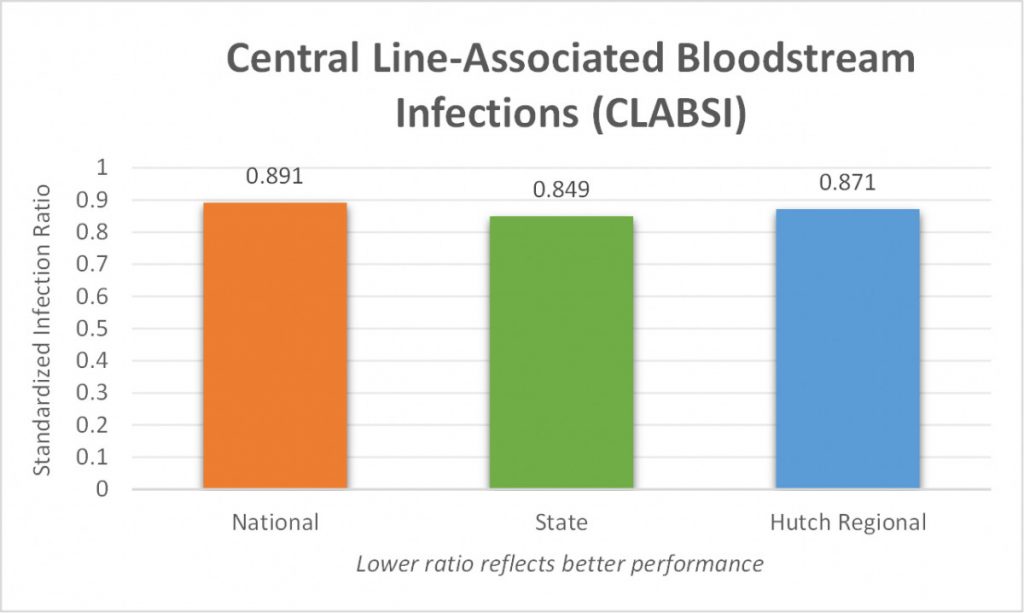
The Standardized Infection Ratio (SIR) is a statistic used to track healthcare associated infections (HAIs) over time, at a national, state, and facility level. The SIR compares the actual number of HAIs at each hospital, to the predicted number of infections.
We follow the recommended central line insertion best practices to prevent infection when the central line is placed, which includes:
We have received your scholarship application. Our team will review your submission, and we will contact you about next steps.
